Table of Contents

Introduction
Fungal acne, also known as Malassezia folliculitis or Pityrosporum folliculitis, is a common skin condition caused by an infection in hair follicles. Often confused with common acne, it presents with distinct symptoms and requires a different approach to diagnosis and treatment. In this comprehensive guide, we will delve into the intricacies of it, exploring its causes, symptoms, diagnostic methods, treatment options, preventive measures, and the overall outlook for individuals dealing with this condition.
An Overview
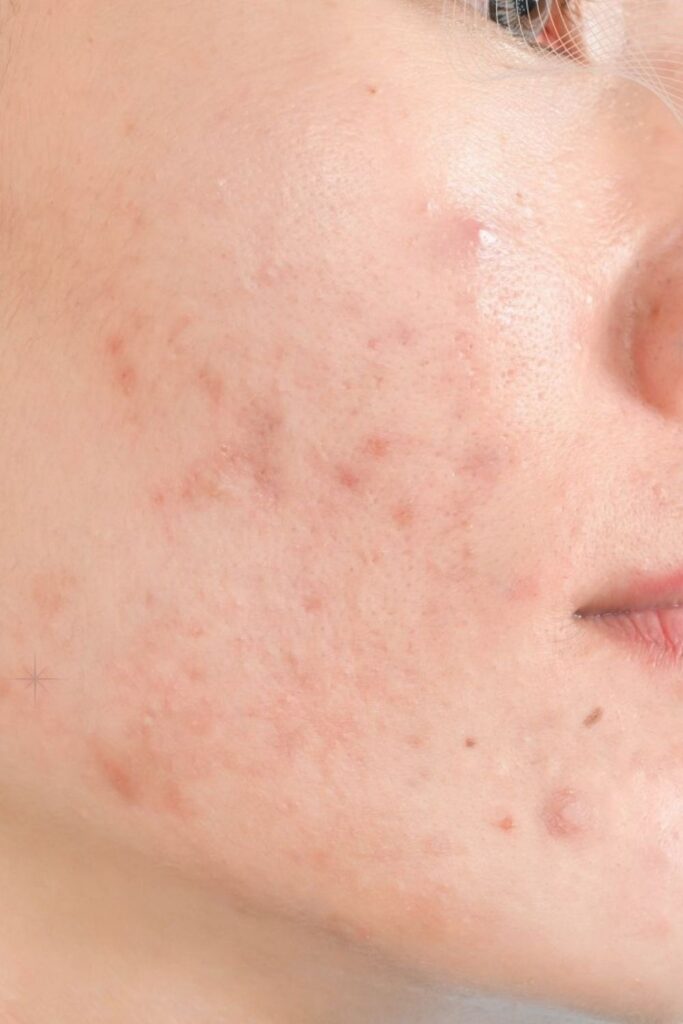
It arises when hair follicles become infected with a fungus called Malassezia yeast. This condition manifests as clusters of small, itchy, red bumps (papules) on the skin. In some cases, these papules can grow larger and evolve into whiteheads, forming small pockets of white or yellow pus (pustules).
Distinguishing Fungal Acne from Common Acne
It is often mistaken for acne vulgaris, which is characterized by the formation of pimples. The key distinction lies in the underlying causes and the presence of itching. Common acne occurs when hair follicles become clogged with bacteria, oil, and dead skin cells, resulting in the development of pimples. In contrast, it is attributed to a fungal infection within the hair follicles and is typically accompanied by itching, a symptom not commonly associated with acne vulgaris.
It is essential to differentiate between fungal and common acne as their treatments differ. However, it is possible for both types of acne to coexist in some individuals.
Who is at Risk of Fungal Acne?
It can affect individuals of all ages, but it is more prevalent among adolescents and young adult males who often have oily skin—a favorable environment for the thriving of yeast. Additionally, factors that increase the risk of developing it include:
- Living in a hot, humid climate: High temperatures and humidity create conditions conducive to the growth of Malassezia yeast.
- Weakened immune system: Individuals with compromised immune systems are more susceptible to fungal infections, including fungal acne.
- Other fungal infections: Conditions like seborrheic dermatitis or tinea versicolor can contribute to the development of fungal acne.
- Excessive sweating (hyperhidrosis): Sweating provides moisture, creating an environment suitable for yeast overgrowth.
- Use of oil-based moisturizers and sunscreens: Certain skincare products can promote the growth of Malassezia yeast.
- Antibiotic use: Antibiotics can disrupt the balance of bacteria on the skin, leading to an overgrowth of yeast and potentially exacerbating fungal acne.

Symptoms and Causes
Understanding the Underlying Causes
Malassezia yeast is naturally present on the skin of almost everyone. However, it becomes problematic when it gains access to hair follicles that are damaged or blocked. These follicles may become compromised due to various factors, including:
- Friction: Skin-to-skin contact, excessive rubbing, or chafing can lead to follicular damage.
- Moisture and heat: Prolonged exposure to hot and humid conditions, as well as perspiration, can contribute to the development of fungal acne.
- Hair removal methods: Shaving, plucking, or waxing can disrupt hair follicles, providing an entry point for the yeast.
- Frequent skin contact: Repeated touching or rubbing of the skin can exacerbate the condition.
- Hot tubs and whirlpools: Sharing these environments can increase the risk of infection.
- Tight clothing: Wearing constrictive garments can create friction and trap moisture, promoting the growth of Malassezia yeast.
Additionally, the use of antibiotics can disrupt the natural balance of bacteria and yeast on the skin. When antibiotics reduce the population of beneficial bacteria, it can lead to an overgrowth of yeast, potentially causing or worsening it.
Symptoms of Fungal Acne
The hallmark symptoms of it include a sudden outbreak of small pimples that may resemble a rash. These papules tend to cluster together and have a consistent size and appearance. Each pimple might be surrounded by a red border or ring.
Individuals with fungal acne may experience the following sensations on their skin:
- Burning: Some individuals report a burning sensation in the affected areas.
- Itchiness: Itching is a common symptom of it and is a significant point of differentiation from common acne.
- Pain: The affected areas may be painful or tender to the touch.
While can occur anywhere on the body, it is most commonly found on the chin, chest, forehead, neck, upper arms, shoulders, and upper back.

Diagnosis and Tests
Diagnosing Fungal Acne
The diagnosis of fungal acne is typically carried out by a primary care physician or a dermatologist, a specialist in skin conditions. To confirm the presence of Pityrosporum folliculitis, healthcare providers employ several diagnostic methods, including:
- Symptom assessment: Physicians inquire about the patient’s symptoms and the duration of their presence.
- Visual examination: Healthcare providers visually inspect the affected skin to assess the appearance of papules, pustules, and other characteristic features of fungal acne.
- Skin sample analysis: In some cases, a sample of the affected skin may be collected and examined under a microscope to identify the presence of Malassezia yeast.
- Wood’s lamp examination: This involves using a small black light (Wood’s lamp) to search for areas on the skin that fluoresce in yellow or green, indicating the presence of the yeast.
Management and Treatment
Treating Fungal Acne
The treatment of Malassezia folliculitis typically involves the use of antifungal medications, either orally or topically. The choice of treatment depends on the severity of the condition and the healthcare provider’s assessment. Here are the primary treatment options:
Oral Antifungal Medications:
- Fluconazole: An effective oral antifungal medication commonly used to treat fungal acne.
- Itraconazole: Another oral antifungal medication that may be prescribed, particularly in cases where fluconazole is ineffective or not well-tolerated.
Topical Antifungal Treatments:
- Antifungal creams: Topical creams containing antifungal agents like econazole or ketoconazole can be applied directly to the affected areas.
- Antifungal shampoos: Some individuals may benefit from using antifungal shampoos, which can be purchased over-the-counter or prescribed by a healthcare provider. Selenium sulfide shampoo, often used for dandruff treatment, is one such option.
In cases where fungal acne does not respond well to standard treatments, photodynamic therapy (PDT) may be considered. PDT combines the use of light and a photosensitizer drug to target and destroy unhealthy cells, including those infected by Malassezia yeast.

Potential Side Effects of Fungal Acne Treatment
While antifungal medications are generally safe and effective, they can sometimes lead to side effects. These may include:
- Gastrointestinal symptoms: Oral antifungal medications can cause diarrhea, nausea, vomiting, and stomach pain in some individuals.
- Liver damage: In rare cases, oral antifungal medications may have adverse effects on the liver. Monitoring liver function during treatment may be necessary.
Prevention
Preventing Fungal Acne
Taking proactive measures to prevent the occurrence or recurrence of fungal acne is crucial. Here are some preventive strategies:
- Showering and changing clothes after exercise: This helps remove sweat and moisture from the skin, reducing the risk of fungal overgrowth.
- Safe hair removal practices: When shaving, plucking, or waxing, ensure proper hygiene to minimize the risk of follicular damage.
- Clean hot tubs and whirlpools: If using these facilities, ensure they are well-maintained and regularly sanitized to prevent contamination.
- Proper care of bathing suits: Wash and thoroughly dry bathing suits between uses to prevent the proliferation of yeast.
- Wear loose clothing: In hot and humid conditions or during exercise, opt for loose-fitting clothing to reduce friction and moisture retention.
For individuals experiencing recurrent fungal acne breakouts, healthcare providers may recommend long-term use of antifungal medications as a preventive measure.
Outlook / Prognosis
Can Fungal Acne Recur?
With appropriate treatment, both topical and oral antifungal options, fungal acne can often be effectively managed. However, even after successful treatment, there is a possibility of recurrence. To mitigate this risk, individuals can consider making hygiene changes and incorporating topical antifungal solutions into their weekly skincare routines, such as using an antifungal shampoo.
Living With Fungal Acne
Relieving the Symptoms of Fungal Acne
While medical treatment is essential for managing fungal acne, there are some home remedies that may help alleviate symptoms and promote healing. These include:
- Warm compresses: Applying warm compresses to the affected areas several times a day can provide relief and aid in the healing process.
- Avoiding follicular damage: Ceasing activities that may damage hair follicles, such as shaving or wearing tight-fitting clothing, for approximately one month can help the skin recover.
Before attempting any home remedies, it is advisable to consult with a physician or dermatologist to ensure they are appropriate for your specific case.
Conclusion
Fungal acne, also known as Malassezia folliculitis, is a skin condition caused by a fungal infection in hair follicles. It differs from common acne in its symptoms, causes, and treatment approaches. Recognizing the signs of fungal acne and seeking appropriate medical care are essential steps in managing this condition effectively.
Individuals dealing with fungal acne can take preventive measures to reduce the risk of recurrence, such as maintaining good hygiene practices and following their healthcare provider’s recommendations for long-term management. With the right treatment and ongoing care, individuals can manage fungal acne and enjoy healthier skin. If you experience persistent itchy breakouts that don’t resolve, consult with a healthcare provider for guidance and treatment options.

Share this content: